What Is A
Root Canal?
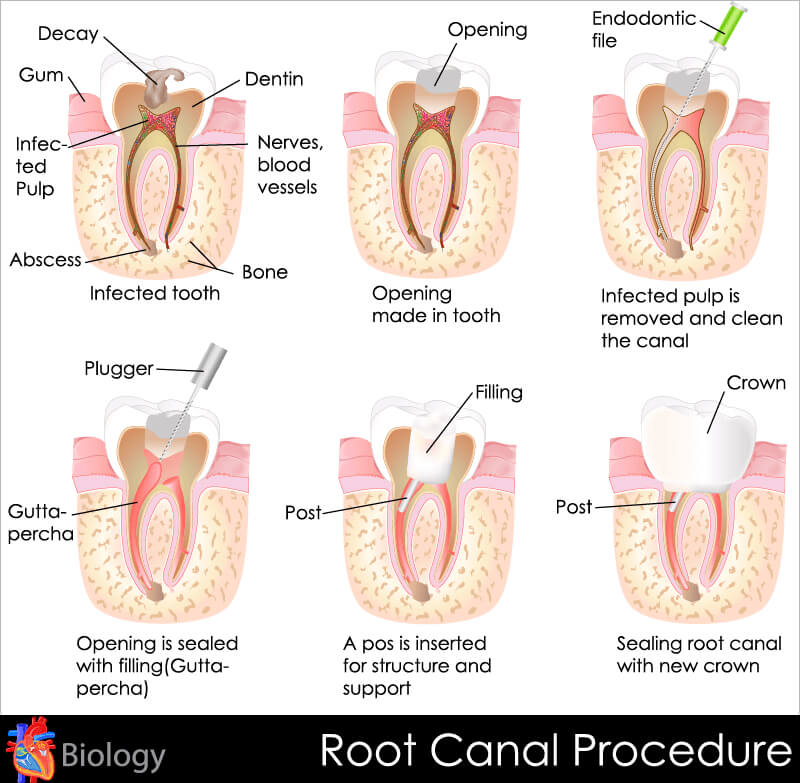
Root canal treatment (endodontic treatment) typically involves the repair of a tooth that is infected or has a dying nerve, with the aim of saving it. It is usually a straightforward procedure that can also help relieve dental pain.
In the traditional clinical setting, root canal procedures were painful but in the modern day setting, technological advances in the dental field ensure that a majority of people experience minimal or no pain at all with the procedure.
A root canal treatment is performed to relieve inflammation and infection in the root of a tooth. In the procedure, the nerve (pulp) is extracted and the dentist then cleans the inside of the tooth, disinfects it and fills it up. Usually 2 or 3 visits are required to complete the treatment. It is important to note that failure to treat such teeth often results in the tooth getting an abscess.

Why Treatment is Vital
Following the damage of the pulp or nerve, a tooth typically begins to break down, subsequently, leading to a proliferation of bacteria that rapidly multiply in the pulp chamber. What follows is that the bacteria and decayed debris result in an abscessed tooth.
The abscess is a pocket filled with pus that forms at the end of the tooth roots resulting in an infection that spreads beyond the roots of a tooth. Usually, the abscess results in bone loss at the root tips, and swelling that can spread to the head, neck, and face. Therefore, root canal treatment is not just about treating pain but it also helps preserve the health of the mouth.
Personal Care After Treatment
Although root canal treatments involve removal of nerves, it is imperative to note that the tooth still has nerve endings that could easily be irritated and inflamed after treatment. It is advisable to chew food on the opposite side of the mouth until the affected area is completely healed. Good oral hygiene and regular checkups are also vital to maintaining a healthy mouth and teeth after such procedures.
We create beautiful smiles with our experienced dental team!
Call us or book your appointment today.
Root Canal FAQs
Which Oral Health Issues Call for a Root Canal?
Your dentist will first examine your teeth to determine if you are a candidate for a root canal. Some people may not even know they have certain signs and symptoms that dentists look for the procedure, such as:
- Severe toothache whenever you chew food
- Sensitivity to cold and hot food or drink even after consuming
- Tooth discolouration or darkening
- Gums tend to be swollen and tender frequently
- Hole in the tooth
- Gum pimple that does not go away
- Swollen neck or face
If you experience one or more of the above, you will likely undergo the therapy.
Will I Lose My Tooth?
The answer will depend on the issue. Most of the time, patients do not need to lose their infected tooth. It is another story if the problem is severe, such as the tooth is badly decayed, and there is no hope to restore the tooth. In such an instance, your dentist may opt to remove the decay and leave the good part intact.
However, it will most likely be covered up with a dental crown or filling. Root canals, in reality, help prevent tooth loss, so it should be something you should not worry about.
Will the Treatment Weaken My Tooth?
Many patients are concerned about the root canals leading to a weakened tooth. The reason is that the nerves inside the tooth are removed through a root canal treatment. Some people think it will affect how the tooth works in the future.
But the good news is that the therapy does not weaken or even kill the tooth because the nerves removed have little to insignificant use. It is why after the completion of the treatment, the function of the tooth will go back to normal, almost as if nothing happened.
Are There Any Complications That I Should Be Aware of?
Root canals are usually successful, and most people experience very negligible effects. However, new infections can appear despite our dentist cleaning and sealing the tooth properly. One reason behind this complication is that there is a crack left undetected in the root of a tooth.
In some cases, root canals can fail, resulting in a defective or inadequate restoration. Bacteria then seep in, leading to re-contamination of the area. If there is inner sealing, it can break down over time. It is why you should always stay in contact with 123 Dental and ensure that you report any issues you encounter.
What Should I Expect After the Root Canal Treatment?
During the first few days, the tooth and the surrounding area may feel a little sensitive because of tissue inflammation. You can take any over-the-counter medication if it is uncomfortable. You may have to minimise chewing on the area while your tooth is still under repair. It helps avoid contamination, which can affect the tooth’s interior and cause fragility.
Once the entire procedure is complete and you have your permanent filling or crown, you can go back to regular chewing. Make sure you brush and floss regularly. Don’t forget to schedule your visits with 123 Dental, as well.
Is There Anything I Can Do to Avoid Root Canal Treatments in the Future?
Absolutely! You may already know that good oral hygiene will present any more future root canal therapies. Apart from brushing and flossing daily, you should also avoid consuming drinks and food high in sugar. Stay away from acidic beverages, as well, including fruit juices and soda. These steps are incredibly easy, but many people fail to follow them, which can lead to tooth decay.
Finally, you should visit 123 Dental at least once a year. That way, our dentist can examine your teeth, and you can have them professionally cleaned.
If I Don’t Want a Root Canal Treatment, What Is a Good Alternative?
One thing that patients should know is that they can say no to any treatment, including a root canal. If you have decided you do not want to go through this therapy, you can opt to have the whole tooth extracted instead. However, we believe that it is better to try saving it first, mostly if the tooth can still be restored. Root canals have a high success rate, and the treatment can prevent other problems from occurring in the future. Some of these issues include teeth shifting, difficulty eating, and jawbone loss.